March 2024
Obesity and the Feet
Obesity is a common problem in American society. Approximately one third of the U.S. population is obese. Obesity is defined as a body mass index greater than 30. Obesity has the power to affect different aspects of the body, and one of the most common problems it causes is foot pain. There have been many studies that found a connection between an increased BMI and foot problems. A simple activity such as walking up a flight of stairs can increase pressure on the ankle by four to six times.
Being overweight causes the body to compensate for the extra weight by changing the way it moves. Consequently, people who struggle with obesity commonly have arch problems in their feet. Obesity causes the arch to break by stretching the ligaments and tendons that hold the bones in the foot together. When the arch lowers, the foot may eventually fall flat. Collapsed foot arches fail to provide adequate shock absorption which eventually leads to foot pain. Other conditions that may be caused by flat feet are pronation, plantar fasciitis, weak ankles, and shin splints.
Foot problems that are caused by obesity may be treated by wearing proper footwear. Proper shoes will allow your feet to have better circulation around the arch and ankle. Additionally, those with obesity often discover that typical heel pain remedies are not effective for them. They will find that their plantar fascia is easily injured, and it is often inflamed. The best way to treat this problem is to implement lifestyle changes. A few good ways to improve your diet are to reduce calories, fill up on fruits and veggies, and to limit sugars.
Custom foot orthotics can prevent foot problems if you’re carrying excess weight or are trying to lose weight. The purpose of orthotics is to provide shock absorption to decrease the amount of stress on the joints to prevent arthritis.
Excess Weight and Circulatory Issues of the Feet

Poor circulation in the feet refers to reduced blood flow to the lower extremities, leading to symptoms like cold feet, numbness, tingling, and slow wound healing. It occurs when blood vessels become narrowed or blocked, restricting the flow of oxygen-rich blood to the feet. Typical causes of poor circulation include peripheral artery disease, atherosclerosis, diabetes, smoking, high blood pressure, and high cholesterol levels. Obesity can exacerbate poor circulation in the feet due to several factors. Excess body weight increases the workload on the heart and blood vessels, leading to conditions like hypertension and atherosclerosis. Fat accumulation around blood vessels can also compress them, further impairing blood flow. Managing poor circulation involves lifestyle changes like regular exercise, maintaining a healthy weight, quitting smoking, and controlling underlying medical conditions. In severe cases, medical interventions like medications or surgical procedures may be necessary to improve blood flow. If you have symptoms of poor circulation in your feet, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment.
The more you weigh, the harder your feet must work to support your body. If you’re an obese individual and are concerned about your feet, contact John Horlebein, DPM from Northern Cascades Foot & Ankle, LLC. Our doctor can provide the care you need to keep you pain-free and on your feet.
Obesity and Your Feet
People who are overweight are putting more pressure on their ankles, knees, and hips as well as their feet. This unfortunately can lead to variety of different issues.
Problems & Complications Stemming from Obesity
- When the body is overweight, it tries to compensate by changing the way that it moves. An obese person may lean forward and put extra weight on the wrong part of the foot. This puts unnecessary stress on the feet.
- Obese people are also more likely to develop type II diabetes which is a condition that causes a lot of foot problems. People with diabetes often don’t feel the cuts and sores that they may have on their feet, which can lead to more complicated and severe issues.
- Plantar fasciitis is another foot condition that can be caused by obesity. Plantar fasciitis is an inflammation of the tissue along the bottom of the foot, which causes pain and stiffness while walking and climbing stairs.
If you have any questions, please feel free to contact our office located in Chelan, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome is a condition in which there is a compression of the posterior tibial nerve. The posterior tibial nerve runs along the inside of the ankle into the foot. Tarsal tunnel syndrome is named for the tarsal tunnel, which is a thin space along the inside of the ankle beside the ankle bones. This space contains various nerves, arteries, and tendons, and includes the posterior tibial nerve. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome the tibial nerve is compressed, causing tingling or burning, numbness, and pain.
Common causes of tarsal tunnel syndrome involve pressure or an injury. Injuries that produce inflammation and swelling in or around the tunnel may place pressure on the posterior tibial nerve. Direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or trauma to the tibial nerve, can result in tarsal tunnel syndrome. Diseases that damage nerves, such as diabetes or arthritis, may cause tarsal tunnel syndrome. Those with flat feet are at risk for developing the condition, as the extra pressure and strain placed on the foot may compress the posterior tibial nerve.
Feeling different sensations in the foot at different times is a common symptom of tarsal tunnel syndrome. An afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg. Symptoms are primarily felt on bottom of the foot and/or the inside of the ankle. Symptoms can appear suddenly and may occur due to overuse of the foot.
To diagnose tarsal tunnel syndrome, your podiatrist may examine the foot and tap the posterior tibial nerve to see if symptoms surface. He or she may also order an MRI to determine if a mass is present.
Treating tarsal tunnel syndrome will depend on the decision of your podiatrist. Multiple options are available, however, and can include rest, ice, immobilization, oral medications such as anti-inflammatory drugs (NSAIDS), physical therapy, injection therapy, orthotics, supportive shoes, braces, and surgery.
What Is Tarsal Tunnel Syndrome?
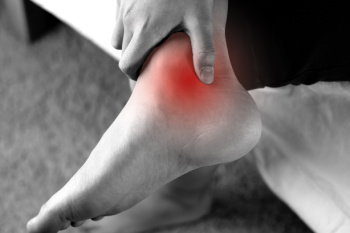 Tarsal tunnel syndrome is a compressive neuropathy condition that results from the entrapment of the posterior tibial nerve as it passes through the tarsal tunnel, a narrow passageway located on the inner side of the ankle. This entrapment leads to many symptoms, most notably pain, tingling, and burning in the foot and heel, which sometimes extends into the toes and lower leg. Many things can cause tarsal tunnel syndrome, such as injuries to the ankle, swelling from other health problems like diabetes, or just by repeating the same movements that irritate the area. Treatment strategies are tailored to the severity and underlying cause of the syndrome. Conservative measures include anti-inflammatory medications and orthotic devices to alleviate pressure on the nerve. More invasive options include surgical decompression to relieve the nerve entrapment. Tarsal tunnel syndrome can be hard to diagnose because its symptoms overlap with other nerve-related conditions. Podiatrists, or foot doctors, can do comprehensive evaluations to properly diagnose tarsal tunnel syndrome. If you have foot pain, or suspect tarsal tunnel syndrome, it is suggested that you seek treatment from a podiatrist who can properly diagnose this condition and offer a personalized treatment plan.
Tarsal tunnel syndrome is a compressive neuropathy condition that results from the entrapment of the posterior tibial nerve as it passes through the tarsal tunnel, a narrow passageway located on the inner side of the ankle. This entrapment leads to many symptoms, most notably pain, tingling, and burning in the foot and heel, which sometimes extends into the toes and lower leg. Many things can cause tarsal tunnel syndrome, such as injuries to the ankle, swelling from other health problems like diabetes, or just by repeating the same movements that irritate the area. Treatment strategies are tailored to the severity and underlying cause of the syndrome. Conservative measures include anti-inflammatory medications and orthotic devices to alleviate pressure on the nerve. More invasive options include surgical decompression to relieve the nerve entrapment. Tarsal tunnel syndrome can be hard to diagnose because its symptoms overlap with other nerve-related conditions. Podiatrists, or foot doctors, can do comprehensive evaluations to properly diagnose tarsal tunnel syndrome. If you have foot pain, or suspect tarsal tunnel syndrome, it is suggested that you seek treatment from a podiatrist who can properly diagnose this condition and offer a personalized treatment plan.
Tarsal tunnel syndrome can be very uncomfortable to live with. If you are experiencing tarsal tunnel syndrome, contact John Horlebein, DPM of Northern Cascades Foot & Ankle, LLC. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tarsal Tunnel Syndrome
Tarsal tunnel syndrome, which can also be called tibial nerve dysfunction, is an uncommon condition of misfiring peripheral nerves in the foot. The tibial nerve is the peripheral nerve in the leg responsible for sensation and movement of the foot and calf muscles. In tarsal tunnel syndrome, the tibial nerve is damaged, causing problems with movement and feeling in the foot of the affected leg.
Common Cause of Tarsal Tunnel Syndrome
- Involves pressure or an injury, direct pressure on the tibial nerve for an extended period of time, sometimes caused by other body structures close by or near the knee.
- Diseases that damage nerves, including diabetes, may cause tarsal tunnel syndrome.
- At times, tarsal tunnel syndrome can appear without an obvious cause in some cases.
The Effects of Tarsal Tunnel Syndrome
- Different sensations, an afflicted person may experience pain, tingling, burning or other unusual sensations in the foot of the affected leg.
- The foot muscles, toes and ankle become weaker, and curling your toes or flexing your foot can become difficult.
- If condition worsens, infections and ulcers may develop on the foot that is experiencing the syndrome.
A physical exam of the leg can help identify the presence of tarsal tunnel syndrome. Medical tests, such as a nerve biopsy, are also used to diagnose the condition. Patients may receive physical therapy and prescriptive medication. In extreme cases, some may require surgery.
If you have any questions please feel free to contact our office located in Chelan, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Wound Care
Diabetics must be wary of all wounds, regardless of depth or size. Diabetes, a chronic disease in which the body cannot properly use glucose the way it normally would, causes various complications that make wounds difficult to heal. Nerve damage or neuropathy will cause diabetics to have trouble feeling the pain of a blister or cut until the condition has significantly worsened or become infected. A diabetic’s weakened immune system can make even the most minor of wounds easily susceptible to infection. Diabetics are also more prone to developing narrow, clogged arteries, and are therefore more likely to develop wounds.
Wounds should be taken care of immediately after discovery, as even the smallest of wounds can become infected if enough bacteria build up within the wound. To remove dirt, wounds should be first rinsed under running water only. Soap, hydrogen peroxide, or iodine can irritate the injury and should be avoided. To prevent infection, apply antibiotic ointment to the wound and cover it with a bandage. The bandage should be changed daily. The skin around the wound may be cleaned with soap.
To prevent further exacerbation, see a doctor—especially if you have diabetes. Minor skin conditions can become larger problems if not properly inspected. As the wound heals, make sure to avoid applying pressure to the affected area.
Treatment of Chronic Diabetic Foot Wounds
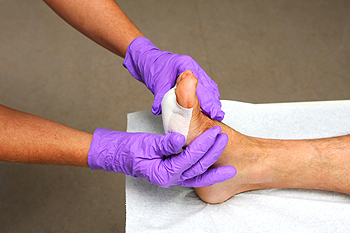
Healing wounds properly involves cells moving and tissue rebuilding in a coordinated way. But in some wounds, like those in diabetes, this process does not work well due to various issues like poor blood flow, infections, and ongoing damage. There's hope for treating such wounds better. By understanding and fixing these issues, following proper care, and using new medical technology, there can be improvement for people with stubborn wounds. If you are diabetic and have chronic foot wounds, it is suggested that you make an appointment with a podiatrist to discuss any new medical technology that might be applied to your case and provide you with relief.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with John Horlebein, DPM from Northern Cascades Foot & Ankle, LLC. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact our office located in Chelan, WA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Foot and Ankle Surgery
When conservative, noninvasive methods prove ineffective, surgery may be selected as the next course of action for the treatment of your foot or ankle condition. A wide number of foot and ankle surgical procedures exist, and it is up to your podiatrist to determine which intervention will be most appropriate and helpful for your case. Some surgical procedures include bunion surgery, fusion, hammertoe surgery, heel spur surgery, metatarsal surgery, nail surgery, neuroma surgery, reconstructive surgery, skin surgery, and tendon surgery. Typically, surgery is turned to as a definitive way to alleviate excessive pain or discomfort and to return your foot to full mobility.
Regardless of the location on the body, all surgical procedures require preoperative testing and examination to ensure the surgery’s success and preferred outcome. A review of your medical history and medical conditions will take place, as will an evaluation of any current diseases, illnesses, allergies, and medications. Tests such as blood studies, urinalyses, EKG, X-rays, and blood flow studies may be ordered. Because the procedure involves the foot and/or ankle, the structures of your feet while walking may also be observed by your podiatrist.
Care post-surgery will depend on the type of surgical procedure performed. Typically, all postoperative care involves rest, ice, compression, and elevation. To improve and ensure a safe recovery, your foot and ankle surgeon may also employ the use of bandages, splints, surgical shoes, casts, crutches, or canes. He will also determine if and when you can bear weight. A timely and thorough recovery is a priority for both you and your podiatrist, and carefully following postoperative instructions can help achieve this.
A Surgical Solution for Bunions
Bunion surgery, medically known as hallux valgus correction, is a procedure aimed at addressing this often painful deformity of the big toe joint. Typically caused by the misalignment of bones, bunions can lead to discomfort, difficulty in shoe-wearing, and decreased quality of life. The surgical process involves making an incision near the affected joint, allowing the surgeon to access and realign the bones and ligaments. In some cases, small screws or plates may be used to secure the corrected alignment. Post-surgery, patients undergo a recovery period during which they are advised to keep weight off the foot and follow a rehabilitation plan. While bunion surgery offers relief from the physical challenges posed by bunions, it is suggested that individuals considering the procedure consult with a podiatrist to determine the most suitable course of action based on their specific condition and overall health.
Foot surgery is sometimes necessary to treat a foot ailment. To learn more, contact John Horlebein, DPM of Northern Cascades Foot & Ankle, LLC. Our doctor will assist you with all of your foot and ankle needs.
When Is Surgery Necessary?
Foot and ankle surgery is generally reserved for cases in which less invasive, conservative procedures have failed to alleviate the problem. Some of the cases in which surgery may be necessary include:
- Removing foot deformities like bunions and bone spurs
- Severe arthritis that has caused bone issues
- Cosmetic reconstruction
What Types of Surgery Are There?
The type of surgery you receive will depend on the nature of the problem you have. Some of the possible surgeries include:
- Bunionectomy for painful bunions
- Surgical fusion for realignment of bones
- Neuropathy decompression surgery to treat nerve damage
Benefits of Surgery
Although surgery is usually a last resort, it can provide more complete pain relief compared to non-surgical methods and may allow you to finally resume full activity.
Surgical techniques have also become increasingly sophisticated. Techniques like endoscopic surgery allow for smaller incisions and faster recovery times.
If you have any questions please feel free to contact our office located in Chelan, WA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.